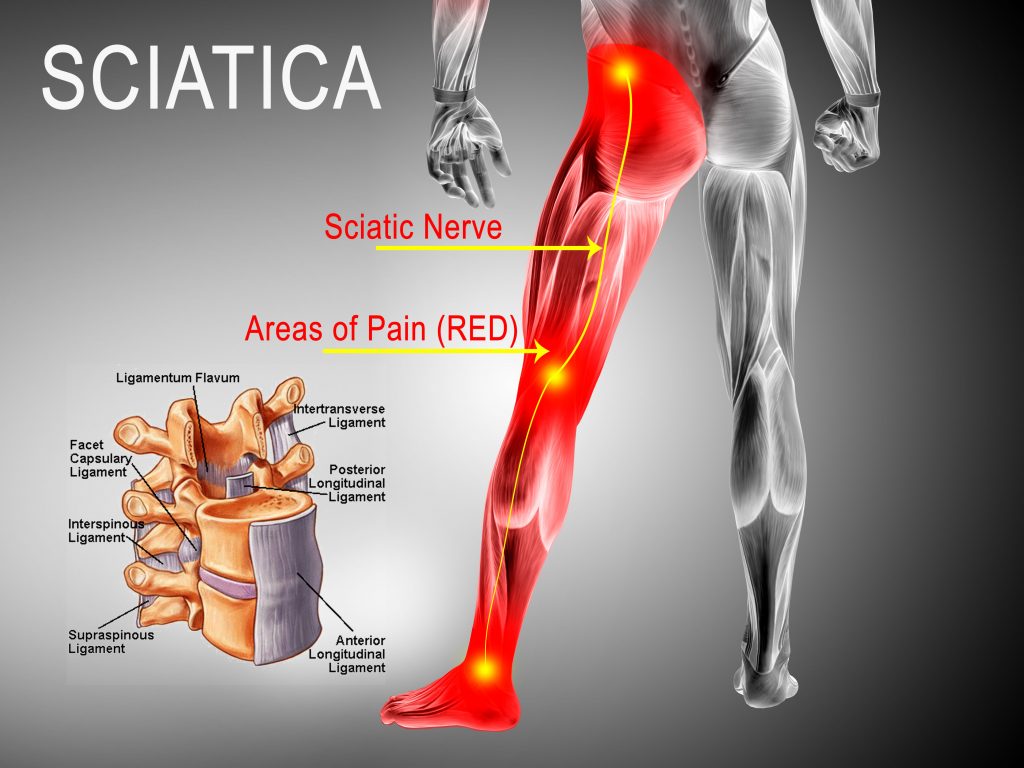
Sciatica
Definition
Sciatica is a symptom, not a disease in itself. It consists of pain in the posterolateral part of the leg that can resemble a cramp. Sometimes it presents as a throbbing pain that makes it impossible to stand or sit. Sciatica can occur suddenly or gradually. The patient also can feel numbness or a tingling sensation that runs down the leg to the foot. Some less common symptoms include the inability to bend the knee or move the foot and toes.
Sciatic pain can be triggered by the slightest movement, such as when bending over to grab something from the floor and it may get worse after standing or sitting, or after walking a long distance. It usually decreases with night rest.
Epidemiology
Sciatica is a very common symptom. It usually affects people between 30 and 50 years of age. There is no exact data on the incidence and prevalence of sciatica, but in general, it is estimated that 5 to 10% of patients with low back pain have sciatica, while the prevalence of low back pain throughout life is 49 to 70%.
Risk factors
Personal factors:
Age (most frequent 45 to 64 years old).
High stature.
Smoking.
Mental stress.
Occupational factors:
Stressful physical activity.
Driving for a long time.
Exposure to vibrations.
Remaining seated for a long time.
Causes
As mentioned above, sciatica is a symptom and can be caused by a wide variety of pathologies that can affect the spine. Among the most frequent we can find:
Herniated disc that causes pressure on the root of the sciatic nerve (this is the most common cause of sciatica).
Piriformis syndrome: it is caused when the piriformis muscle tenses or suffers a spasm, compressing the sciatic nerve in its passage through the greater sciatic foramen.
Lumbar stenosis: this condition results from the narrowing of the lumbar canal that puts pressure on the nerves (represents the most common cause in people over 60 years).
Spondylolisthesis: it is a sliding of a vertebra so that it is misaligned with the vertebra immediately superior, narrowing the channel through which the nerve passes.
Diagnosis
A complete medical history, including a detailed explanation of symptoms and a full physical examination can help the doctor diagnose sciatica and determine its causes. The physical examination depends mainly on the neurological signs. The most useful sign is obtained with the maneuver of Lasègue, which consists of raising the leg of the patient while keeping the knee extended. When performing this movement, the roots of the sciatic nerve stretches and produces pain.
Imaging studies are useful to determine the cause of sciatica, the most used are:
Anteroposterior and lateral spine radiography: allows identifying structural alterations such as osteoarthritis, spondylolisthesis, lumbar stenosis, etc.
Magnetic resonance imaging (MRI) or computerized axial tomography (CT): allows better visualization of the intervertebral discs.
Electromyography: it allows evaluating the electrical activity of the affected muscles.
Treatment
The goal of treatment is to decrease pain and increase mobility. Treatment usually includes rest, physical therapy, and the use of medications to decrease pain and inflammation.
Pharmacotherapy:
Analgesics and nonsteroidal anti-inflammatory drugs (NSAIDs) help relieve pain and stiffness, increasing mobility. Muscle relaxants are indicated to relieve the discomfort associated with muscle spasms. Spinal infiltrations with the injection of steroids in the lower back can help reduce the inflammation of the nerve roots, allowing the patient to have an increase in mobility.
Physiotherapy:
The goal of physical therapy is to find exercises that can decrease the pain of sciatica by reducing the pressure on the nerve. An exercise program usually includes stretching exercises to improve the flexibility of tense muscles and aerobic exercises, such as walking. The therapist can also recommend exercises to strengthen the muscles of your back, abdomen and legs.
Surgery:
The procedure to be performed depends on the pathology that causes the sciatica. Is indicated in those patients who do not respond to conservative treatment, or those who have severe symptoms and motor deficit.
Prevention
You can perform certain activities that reduce the risk of developing sciatica:
Use appropriate lifting techniques. Raise your right back, and get up with your hips and legs, and holding the object as close to your chest as possible.
Stop smoking cigarettes, as it promotes disc degeneration.
Exercise regularly to strengthen your back and abdomen muscles, which support your spine.
.jpg)
Have a good posture when standing, sitting or sleeping. Having a good posture can help relieving the pressure of your lower back.
Try not to be seated for long periods of time.
.jpg)
