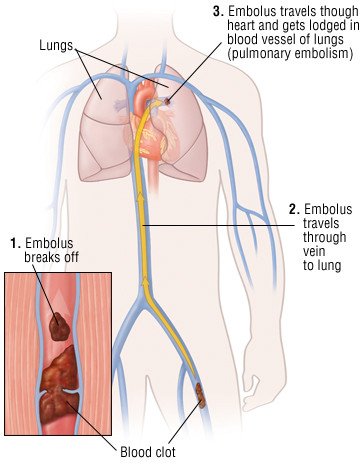
A deep venous thrombosis (DVT) is a blood clot (thrombus) that forms inside deep veins in your legs or pelvis. The clot blocks blood flow and causes pressure to build up in the vein. Part of the clot can break away and move through your bloodstream to your lungs. If the clot blocks one or more of the blood vessels in your lungs, it is called a pulmonary embolism.
DVT is a common problem. Most of these clots occur when blood flow in the veins of the legs is slowed. This is usually as a result of inactivity.
Ordinarily, as you walk around, your leg muscles squeeze your veins and keep blood flowing back to the heart. But if you are inactive for many hours, blood flow in the veins of your legs may slow so much that clots form. Long periods of inactivity can occur during a long airplane flight or while recovering from an operation or stroke, for example.
Certain people are more likely to get blood clots. These include:
- People with some medical problems, including cancers and inherited abnormalities of the blood-clotting system
- People on certain medications, such as birth control pills and hormone therapy
- Pregnant women
- People who are very overweight
- People with heart failure
Anyone who develops DVT is at risk of developing a pulmonary embolism.
A pulmonary embolism can lead to a sudden and sometimes very dramatic decrease in blood flow through the lungs. The decrease in blood flow can reduce the amount of blood flowing to your heart and the rest of your body. This can cause a drop in blood pressure and lead to fainting spells and even sudden death.
The blood flow decreases in part because the blood clot blocks blood flow. In addition, the blockage damages the walls of the lung's blood vessels. The damage releases chemicals that cause blood vessels to narrow.
Symptoms
Some blood clots in the leg veins do not cause any symptoms. However, when the blood clots involve larger veins, they generally cause:
- Leg pain and tenderness
- Swelling (edema)
- A sensation of heaviness in the leg, particularly when you've been standing
You can check for edema by pressing your finger into your lower leg. If you have edema, the pressure from your finger will create a small dent in your lower leg for several seconds.
A pulmonary embolism may cause no symptoms, mild symptoms, or serious symptoms that indicate a life-threatening emergency. Symptoms tend to be more severe when the blood clot is larger.
Symptoms with a larger clot include sudden shortness of breath and chest pain. The pain tends to be knife-like. It often is worse when you take deep breaths.
If the pulmonary embolism is very large, symptoms may be more dramatic. They may include fainting spells, severe shortness of breath, and coughing up blood. A large pulmonary embolus can cause sudden death.
Diagnosis
To diagnose DVT, your doctor will examine your legs to check for swelling and tenderness. He or she will ask about your symptoms and risk factors.
Based on the findings, your doctor may order a D-Dimer blood test or an ultrasound of your legs.
The blood test measures the level of a chemical called D-Dimer. It is almost always abnormally high when blood clots are actively forming in the body.
An ultrasound of your legs is done to look for blood flow problems in your veins. This procedure is called a lower extremity non-invasive test, or LENI. If the LENI shows evidence of a blood clot, your doctor will diagnose DVT.
If the initial LENI is negative, it does not mean that there is no clot. It may be too early to see the full effect of the clot. Your doctor may ask that you return in three to four days for a repeat LENI.
If your doctor suspects you have a pulmonary embolism, he or she will first try to determine if you have DVT. If the LENI shows one or more blood clots in your leg veins, and you have symptoms of a pulmonary embolism, an embolism is the most likely diagnosis.
Or your doctor may order computed tomography (CT) of the chest. The test requires an IV injection of dye to look for blood clots in the pulmonary arteries. People that have impaired kidney function or an allergy to the dye might need a different type of lung scan called a V/Q scan to examine lung blood flow.
Expected Duration
If you have a DVT or pulmonary embolism, your symptoms should improve within a few days after starting treatment with blood-thinning medication. You will need to take medication for at least three to six months to prevent more blood clots from forming.
Most people recover completely. But some people who had a very large pulmonary embolism or who already had lung disease will continue to have lung problems.
Some people who have had a DVT develop a long-term problem with swelling of their legs. This is called post-phlebitic syndrome. These people often need to wear special stockings that help squeeze blood back toward the heart.
Prevention
Most DVTs and pulmonary embolisms develop in people who are inactive because of an injury or surgery.
If you have had a DVT or pulmonary embolism, or you have a family history of blood-clotting problems, you can help prevent blood clots. Do the following:
- Ask your doctor if you have any risk factors for blood clots that can be changed.
- Avoid all medications that may cause blood clots. These include birth control pills and other medications that contain estrogen.
- Drink a lot of water and walk around frequently when on long plane flights or car trips.
- Avoid prolonged periods of bed rest.
- Discuss your history of DVT and pulmonary embolism with your physician before considering any surgical procedures.
Treatment
The initial treatment for a DVT or pulmonary embolism is heparin or one of the new novel oral anti-coagulant drugs. These medications act on certain blood proteins to prevent new blood clot formation and therefore help unwanted clots get smaller. They are commonly called "blood thinners."
There are two main types of heparin. The oldest type of heparin is best administered by a constant intravenous infusion. Another type of heparin is called low-molecular-weight heparin. It is injected under the skin once or twice per day.
Some of the newer anti-coagulant drugs are approved for initial treatment of DVT and pulmonary embolism. Examples include rivaroxaban (Xarelto) and apixaban (Eliquis).
If you have a DVT without a pulmonary embolism, you may not need to be hospitalized. You could be treated at home with injections of a low-molecular-weight heparin or either rivaroxaban or apixaban.
Some people may need to start therapy in the hospital. In this case, the type of heparin used is determined by many factors. These include body weight, kidney function and other circumstances.
If you have a pulmonary embolism, you will probably be hospitalized. If so, you likely will be treated with either type of heparin initially. But oral rivaroxaban or apixaban could be an option instead of heparin if your pulmonary embolism is small.
If you are started on either IV heparin or low-molecular weight heparin shots under the skin, your doctor will transition you to an oral drug. Traditional oral therapy has been warfarin (Coumadin). For decades, it was the only oral drug to treat DVT and pulmonary embolism.
Today, in addition to rivaroxaban and apixaban, another novel oral anti-coagulant can be used after heparin. It's dabigatran (Pradaxa). More of these types of drugs will be approved soon.
Warfarin takes a few days to start working. Once a blood test shows that warfarin is effective, you will stop taking heparin. You will continue taking warfarin for several months or longer.
During the first few weeks that you take warfarin, you will continue to need frequent blood tests to make sure you are taking the right amount. Once your blood test results consistently show that you are taking the right amount of medication, blood can be drawn every two to four weeks.
Some foods—especially green, leafy vegetables that contain large amounts of vitamin K—can alter the blood-thinning action of warfarin. Ask your doctor or pharmacist for a list of these foods. You can continue to eat these foods as long as you eat approximately the same amount of them each day. That way, the effect on your medication will be consistent.
Other medications can also affect how warfarin works in your body. Tell any doctor who is prescribing medications for you that you are taking warfarin.
The new novel oral anti-coagulants don't require regular blood testing. They are given in a fixed dose. The other advantage is not worrying about eating food with too much vitamin K.
When To Call a Professional
Call your doctor or go to a hospital emergency room immediately if you develop shortness of breath or sharp chest pain.
Call your doctor if you have new unexplained onset of swelling and pain in one leg.
Even if you are scheduled for a repeat LENI test in three or four days, call your doctor sooner if your leg swelling worsens.
Prognosis
Without treatment, a pulmonary embolism can be deadly. With appropriate and timely treatment, the outlook is very good.
Once you develop a DVT or pulmonary embolism, you are usually more likely to develop a second blood clot. This is because the original blood clot damages some of your leg veins. Now, your blood does not move as quickly or smoothly through these veins. This increases your risk of a new blood clot.
However, if there is a clear reason that the blood clot formed, such as a long bed rest after surgery or an injury that damaged your blood vessels, your risk of developing more blood clots is relatively low unless you are forced to be inactive again or have another injury.
