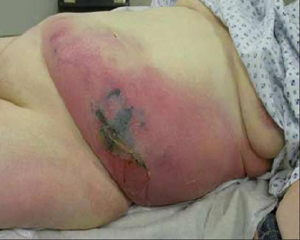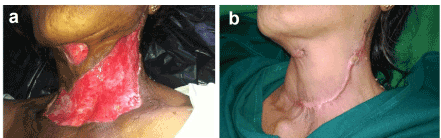
Necrotizing fasciitis is a rare bacterial infection that spreads quickly and destroys skin, fat, and muscle. It is also known as flesh-eating bacteria. Necrotizing fasciitis is a life-threatening infection that must be treated immediately.
What causes necrotizing fasciitis?
Necrotizing fasciitis is caused by bacteria commonly found on your skin or in your throat. The bacteria enter the body through a break in the skin, such as a bug bite, scrape, or burn. In most people, the bacteria do not cause a serious infection. People with weak immune systems or chronic medical conditions have an increased risk for necrotizing fasciitis.
Having a weakened immune system and certain diseases may make you more likely to get flesh-eating bacteria (necrotizing fasciitis). Health conditions that may raise your risk include:
- Alcohol abuse
- Cancer
- Chickenpox (in childhood)
- Cirrhosis
- Diabetes
- Heart disease affecting the heart valves
- Chronic kidney disease
- Lung disease, including tuberculosis
- Peripheral vascular disease
- Steroid use
- Use of injectable or IV drugs
What are the signs and symptoms of necrotizing fasciitis?
- Redness, swelling, and severe pain
- Sores or blisters that ooze
- Flu-like symptoms, such as fever, chills, nausea, and muscle pain
- Fatigue, lightheadedness, and fainting
The early symptoms of an infection with flesh-eating bacteria usually appear within the first 24 hours of infection. Symptoms are similar to other conditions like the flu or a less serious skin infection. The early symptoms are also similar to common post-surgical complaints, such as:
- Serious pain
- Inflammation
- Fever
- Nausea
Symptoms often include a combination of the following:
- Increasing pain in the general area of a minor cut, abrasion, or other skin opening.
- Pain that is worse than would be expected from the appearance of the cut or abrasion.
- Redness and warmth around the wound, though symptoms can begin at other areas of the body.
- Flu-like symptoms such as diarrhea, nausea, fever, dizziness, weakness, and general malaise.
- Intense thirst due to dehydration.
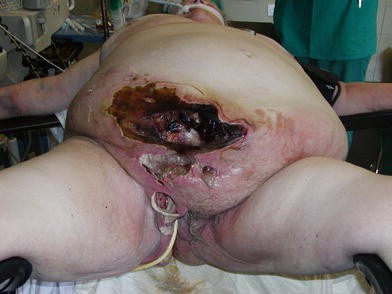
More advanced symptoms happen around the painful infection site within 3 to 4 days of infection. They include:
- Swelling, possibly along with a purplish rash
- Large, violet-colored marks that turn into blisters filled with dark, foul-smelling fluid
- Discoloration, peeling, and flakiness as tissue death (gangrene) happens
Critical symptoms, which often occur within 4 to 5 days of infection, include:
- A severe drop in blood pressure
- Toxic shock
- Unconsciousness
How is necrotizing fasciitis diagnosed?
- Blood tests are done to check for signs of infection and inflammation.
- A tissue culture of your wound is done to find the type of bacteria that is causing your infection.
- An x-ray, CT scan, or MRI may help show where the infection has spread. You may be given contrast liquid to help the pictures show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
How is necrotizing fasciitis treated?
- Medicines help treat your infection and reduce your pain.
- Surgery may be needed to remove dead tissue and help prevent the spread of your infection. You may need surgery to relieve pressure, or a skin graft to reconstruct the infection site. Limb amputation may be needed to save your life.
- Hyperbaric therapy may be used to decrease swelling and increase wound healing.
- Wound vacuum therapy may be used to help stop bacteria from spreading and increase wound healing.
How can I prevent another infection?
Wash your hands often. Wash your hands several times each day. Wash after you use the bathroom, change a child's diaper, and before you prepare or eat food. Use soap and water every time. Rub your soapy hands together, lacing your fingers. Wash the front and back of your hands, and in between your fingers. Use the fingers of one hand to scrub under the fingernails of the other hand. Wash for at least 20 seconds. Rinse with warm, running water for several seconds. Then dry your hands with a clean towel or paper towel. Use germ-killing gel if soap and water are not available. Do not touch your eyes, nose, or mouth without washing your hands first.
Washing your hands with soap and water or using an alcohol-based hand sanitizer is one of the best steps you can take to prevent flesh-eating bacteria and other skin infections.
- You can also prevent skin infections by taking these steps:
- Always clean cuts and open wounds with soap and water.
- After cleaning, cover an oozing, draining, or open wound with a clean, dry bandage.
- Get treated by a doctor if you have a serious or deep wound, such as a puncture or gunshot.
- Don’t go swimming or use a hot tub if you have an open wound or skin infection.
- Clean all wounds immediately. Use soap and water to clean even small breaks in your skin, such as minor cuts or blisters. Cover the wounds with a sterile bandage. Change the bandage as directed or if it becomes wet or dirty.
- Limit your exposure to bacteria. Avoid people who are sick and have a sore throat. The bacteria that cause strep throat can also cause necrotizing fasciitis.
When should I seek immediate care?
- You have a fever and a new wound with redness, swelling, or pain.
- You have flu-like symptoms within 24 hours of an injury.
- You have dark blisters near your wound that drain black fluid.
- The area around your wound is numb.
- The skin around your wound becomes discolored or flaky.
Flesh-Eating Bacteria Treatment:
Patients infected with flesh-eating bacteria will undergo several types of treatment. The extent of treatment depends on the stage of the disease when treatment is started. The treatment includes:
- Intravenous antibiotic therapy.
- Surgery to remove damaged or dead tissue in order to stop the spread of infection.
- Medications to raise blood pressure.
- Amputations of affected limbs, in some cases.
- Hyperbaric oxygen therapy may be recommended to preserve healthy tissue.
- Cardiac monitoring and breathing aids.
- Blood transfusions.
- Intravenous immunoglobulin. This supports the body's ability to fight infection.
Flesh-Eating Bacteria Complications
Serious complications are common and may include:
- Sepsis
- Shock
- Organ failure
- Loss of an arm or leg due to amputation
- Severe scarring
- Death
When should I call my doctor?
- You have a sore throat.
- You have questions or concerns about your condition or care.
Flesh-Eating Bacteria Outlook
Early diagnosis and rapid, aggressive treatment are critical when it comes to fighting this rare skin infection. Many people need more than one procedure to remove damaged, infected tissue. If you have red, swollen skin and it’s not going away, make an appointment with your doctor.